When decay or a small fracture weakens a tooth, a carefully placed filling restores its shape and function so you can chew, speak, and smile without discomfort. Fillings are one of the most common restorative procedures because they preserve natural tooth structure and prevent problems from progressing.
Modern restorative dentistry focuses on conservative repairs that maintain as much healthy tooth as possible. Rather than simply "patching" a tooth, contemporary techniques aim to rebuild strength, seal against future decay, and deliver an outcome that looks and feels natural.
Our team approaches each restoration with precision and patient comfort in mind. At Lorber Dental NY, PLLC, we combine diagnostic imaging, careful preparation, and proven materials so your restoration supports long-term oral health while blending seamlessly with your smile.
Humans have worked to fix damaged teeth for millennia. Early attempts at dental repair show a long history of inventive approaches, and over time clinicians and material scientists have refined those efforts into the reliable restorations used today.
The 19th and 20th centuries introduced strong metal restoratives such as gold and amalgam, valued for durability. In recent decades, however, dental materials have evolved to meet both functional and aesthetic demands, giving patients more attractive, biocompatible options that preserve tooth structure.
These newer materials—designed to bond with tooth surfaces, resist wear, and match natural color—allow dentists to deliver restorations that are durable without drawing attention. Improvements in adhesive technology and ceramic systems have broadened the ways we can repair teeth with predictable, long-lasting results.
Every patient and every tooth is unique. That’s why treatment planning begins with a thorough exam and a clear conversation about your needs, priorities, and the health of the surrounding teeth and gums. We tailor restorations to the specific circumstance—whether the priority is maximum strength, a seamless cosmetic match, or a balance of both.
Our team takes time to explain the options available for a particular tooth and what you can expect from each approach. We consider the size and location of the cavity, your bite, aesthetic preferences, and any other dental work that might affect the outcome.
Comfort and clarity are central to our process. We use modern local anesthetics and techniques to minimize discomfort, and we review aftercare and follow-up so you feel confident about the health and longevity of your restoration.
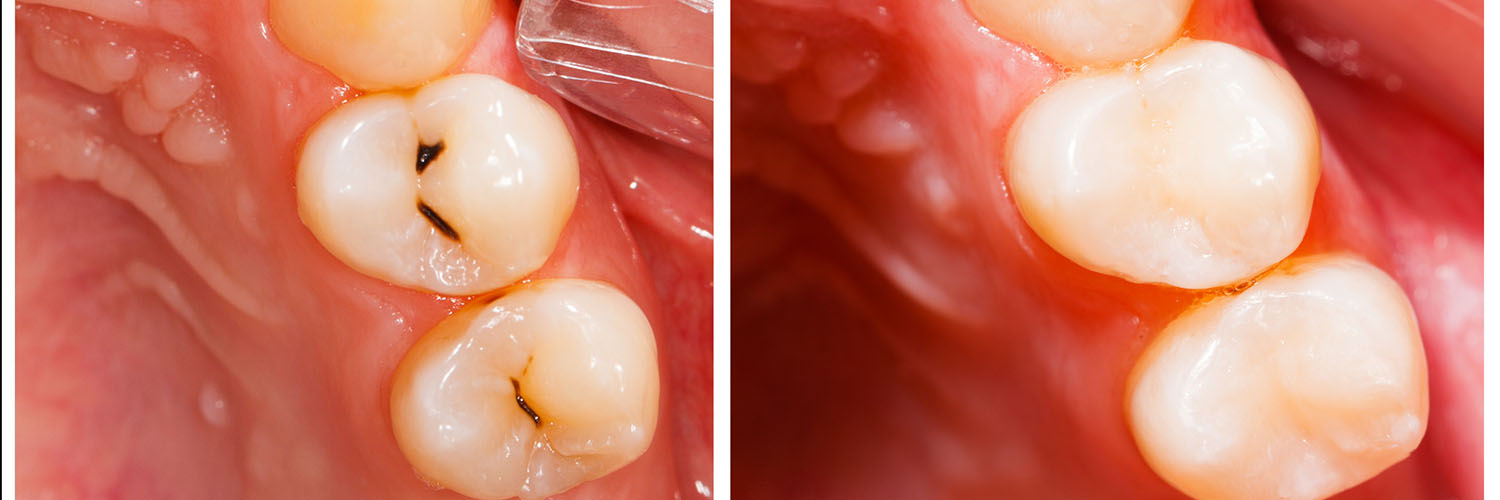
Choosing a filling material involves balancing strength, longevity, appearance, and how much natural tooth must be removed to place the restoration. Advances in dental materials now allow clinicians to select options that closely mimic the tooth’s natural properties.
Below is an overview of commonly used restorative materials and the situations in which they frequently perform best. Your dentist will recommend the material that meets both functional needs and aesthetic expectations.
Composite fillings are resin-based materials that bond directly to the tooth. Available in a variety of shades, they are shaped and cured to match the surrounding enamel, making them a popular choice for visible areas of the mouth.
Because composites adhere to tooth structure, less healthy tooth typically needs to be removed during preparation. They offer an attractive, conservative solution for many cavities, though they may require replacement sooner than some indirect restorations in high-wear areas.
Amalgam has a long history of use due to its toughness and resilience in the back teeth. It can stand up well to heavy chewing forces and has been a reliable option where durability is the top priority.
Though less commonly chosen for front teeth because of its metallic appearance, amalgam remains an effective restorative material for certain clinical situations where longevity and strength are the main concerns.
Glass ionomer materials bond chemically to tooth tissue and release small amounts of fluoride over time, which can be helpful in slowing recurrent decay. They are often used for pediatric restorations, small repairs near the gumline, or as provisional restorations.
While not as wear-resistant as some other materials, glass ionomers are valuable when adhesion and fluoride release are desired features, especially in less stress-bearing areas.
Ceramic restorations—fabricated outside the mouth and cemented or bonded in place—offer excellent color stability and wear resistance. Because they recreate the tooth’s contours precisely, ceramics are ideal for larger restorations where aesthetics and long-term performance are important.
These indirect restorations protect remaining tooth structure and can provide a highly natural appearance, particularly on teeth that receive significant attention during smiling and chewing.
Gold restorations, although less common today, provide superb fit, durability, and biocompatibility. They are often used in cases that prioritize longevity and tissue friendliness, especially when other options are not suitable.
Because gold is a premium material with distinctive appearance and handling characteristics, it is chosen selectively when its advantages align with a patient’s clinical and personal preferences.
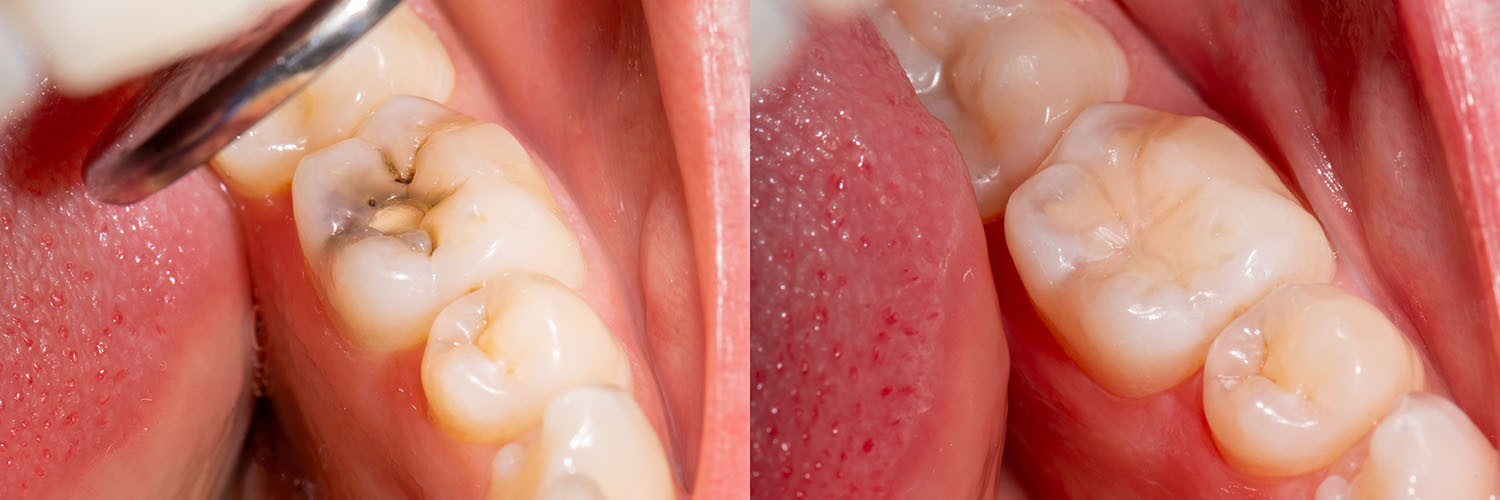
A typical filling appointment starts with a careful assessment: diagnostic X-rays as needed, a clinical exam, and a discussion of the recommended approach. You’ll be informed about the steps involved and what type of restoration is most appropriate for the tooth in question.
Most restorations are completed in a single visit. After numbing the treatment area, the dentist removes the decayed or weakened tissue using rotary instruments, air abrasion, or lasers when clinically appropriate. The goal is to eliminate disease while preserving as much healthy tooth as possible.
Placement techniques vary by material. Direct restorations, like composites and glass ionomers, are placed and cured in the mouth during the same appointment. Indirect restorations, such as ceramic inlays, are fabricated in a lab or by a dental milling unit and fitted at a follow-up visit. If necessary, a temporary restoration may be used between appointments.
Patient comfort is a priority. Local anesthesia is typically sufficient for routine fillings, and we also offer dental sedation options for patients who prefer additional support during treatment. After placement, the bite will be checked and adjusted so the restoration feels comfortable and functions properly.
Proper care after a filling helps extend its life and maintain tooth health. For the first few hours after treatment you may notice numbness; avoid chewing until full sensation returns to reduce the risk of biting your lips or tongue.
It is common to experience mild sensitivity to temperature or pressure for a few days after a filling. This usually resolves on its own. If discomfort persists or worsens, contact the office so we can evaluate the restoration and its surroundings.
Good daily oral hygiene—brushing twice, flossing once, and keeping routine professional cleanings—helps prevent new decay at the margins of a restoration. Regular dental exams allow early detection of wear or recurrent decay so repairs can be made before a small problem becomes larger.
Protect the treated area while numb
Until anesthesia wears off, be careful with hot beverages and avoid chewing on the treated side to prevent accidental injury.
Expect short‑term sensitivity
Mild sensitivity to hot, cold, or pressure can occur for several days; this typically subsides. If you notice persistent pain, contact the office for an evaluation.
Maintain excellent oral hygiene
Cleanings, consistent brushing, and flossing reduce the chance of recurrent decay and help your filling last as long as possible.
Watch for changes over time
Fillings may need repair or replacement after years of service. Addressing changes early helps protect the remaining natural tooth.
We believe clear information and careful technique lead to better outcomes. If you have questions about the type of filling recommended for you or about what to expect before, during, and after treatment, our team is here to help.
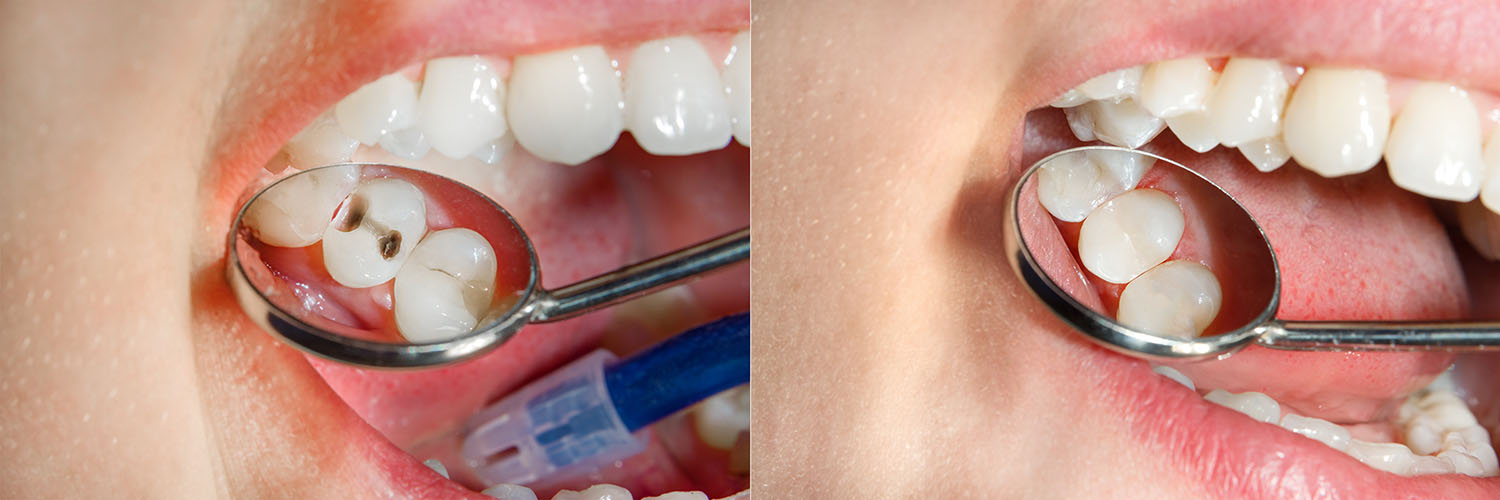
In summary, fillings are a cornerstone of conservative dental care: they remove disease, restore form and function, and help teeth remain healthy for years. If you’d like more information about the materials or techniques described here, or to discuss which option is best for your smile, please contact us for more information.
Dental fillings are restorations that repair areas of tooth structure damaged by decay or small fractures so the tooth can function normally. They restore the tooth's shape and chewing surface while sealing the area to limit further bacterial invasion. Fillings are one of the most common conservative treatments because they preserve as much natural tooth as possible and help prevent more extensive problems.
The decision to place a filling follows a clinical exam and any necessary X-rays to determine the size and location of the lesion. Modern techniques focus on removing the disease while conserving healthy enamel and dentin. The overall goal is to return the tooth to comfortable function and a natural appearance when appropriate.
A range of materials is available for dental fillings, each with advantages and trade-offs that influence clinical choice. Tooth-colored composite resins bond to the tooth and offer excellent aesthetics for visible areas, glass ionomer cements chemically bond and release fluoride, traditional amalgam provides long-standing strength in back teeth, and ceramic or gold restorations are used when durability and precise fit are priorities. The selection depends on factors such as the size of the defect, location in the mouth, aesthetic needs, and expected chewing forces.
Composites typically require less removal of healthy tooth and are matched to enamel shades, but they may wear faster in very large restorations. Glass ionomers are useful in situations where fluoride release or chemical bonding is helpful, such as pediatric care or near the gumline. Indirect options like ceramic inlays and onlays are fabricated outside the mouth to recreate tooth contours precisely and can offer superior longevity and color stability for larger cavities.
A typical appointment begins with a focused exam and any diagnostic imaging needed to confirm the extent of decay or damage. After discussing material options and answering your questions, the treatment area is numbed with local anesthetic to ensure comfort, and the dentist removes decayed or weakened tissue using rotary instruments, air abrasion, or lasers when indicated.
Direct restorations such as composite and glass ionomer fillings are placed and cured in a single visit, shaped to the tooth, and adjusted for a comfortable bite. For larger or indirect restorations like ceramic inlays, impressions or digital scans are taken and a lab-fabricated restoration is fitted at a follow-up visit, with a temporary placed if necessary. At Lorber Dental NY, PLLC, we emphasize clear communication and gentle techniques to make the process predictable and as comfortable as possible.
Tooth-colored composite fillings have improved substantially and can be very durable for small to moderate-sized cavities, especially when placed correctly and maintained with good oral hygiene. Composites bond to the remaining tooth and preserve more structure, which can strengthen teeth that would otherwise need greater removal for a metal restoration. In high-stress areas with heavy chewing forces or when a large portion of the tooth is missing, other options such as ceramic inlays, onlays, or metal restorations may be more appropriate.
Amalgam and gold restorations have a long track record for toughness and wear resistance, particularly in posterior teeth subjected to strong occlusal loads. However, modern adhesive materials and ceramic systems have narrowed the performance gap for many clinical situations. The dentist will recommend the best material by balancing longevity, aesthetics, and how much healthy tooth must be removed.
After a filling, you may experience mild sensitivity to hot, cold, or pressure for a few days; this typically resolves as the tooth settles. Until the local anesthetic wears off, avoid chewing on the treated side to reduce the risk of biting soft tissues or damaging the restoration. Over-the-counter pain relievers and avoiding very hot or cold foods can help manage transient discomfort.
Long-term care focuses on excellent daily oral hygiene—brushing twice, flossing once daily, and maintaining routine professional cleanings—to prevent new decay at restoration margins. Regular dental exams let the dentist monitor wear, contact points, and the integrity of the filling so any needed repairs are identified early. If sensitivity or pain persists beyond a few days, contact the office for an evaluation.
Fillings can fail over time due to wear, fracture, recurrent decay at the margins, or changes in the bite that place uneven forces on the restoration. Small defects such as minor chipping or marginal breakdown may be repaired conservatively, while more extensive problems can require replacement of the filling or escalation to an inlay, onlay, or crown. Regular examinations and X-rays help detect early changes so the least invasive option can be chosen.
Other signs that warrant evaluation include persistent sensitivity, roughness when running your tongue over the filling, or a noticeable change in how your teeth come together. Addressing issues promptly helps protect the remaining natural tooth and reduces the likelihood of more complex treatment in the future.
It is common to have short-term sensitivity after a filling as the pulp of the tooth adjusts to the procedure and the restorative material. This sensitivity typically diminishes within days to a few weeks, but persistent or worsening pain should be evaluated to rule out high contact points, incomplete removal of decay, or nerve involvement. Most patients do not experience long-term adverse effects from commonly used dental materials.
True allergic reactions to dental restorative materials are uncommon but can occur in rare cases; documented sensitivities are more often related to certain metals or components in older materials. If you have a known material sensitivity or significant medical allergy history, tell your dentist so they can select biocompatible alternatives and, if needed, arrange testing or consultation with a specialist.
Pediatric patients and people with high caries risk may benefit from materials and techniques designed to protect vulnerable teeth and reduce recurrent decay. Glass ionomer cements are frequently used in these situations because they bond chemically to tooth structure and release fluoride, which can help slow new decay. For primary molars or very extensive decay in children, stainless steel crowns are a durable option that preserves function until the permanent tooth erupts.
In addition to material choice, individualized preventive strategies such as topical fluoride, sealants on susceptible chewing surfaces, and more frequent recall visits are important in high-risk cases. The clinician will tailor treatment and recall intervals based on age, cavity pattern, oral hygiene, and other health factors to prioritize long-term dental wellness.
The decision hinges on how much healthy tooth remains, the location and size of the defect, and the functional demands on the tooth. Small to moderate cavities that preserve sufficient tooth structure are well suited to direct fillings, while larger defects that compromise cusps or require greater structural support are better treated with indirect restorations like inlays, onlays, or crowns. These lab-fabricated options distribute chewing forces more evenly and can protect the tooth from fracture over time.
Other factors in the decision include aesthetic goals, the patient's bite and parafunctional habits, and the condition of adjacent restorations. A careful clinical exam and diagnostic imaging allow the dentist to recommend the most conservative yet durable option tailored to the tooth's long-term prognosis.
Effective preventive care is the foundation for minimizing the need for restorative treatment by addressing the factors that cause decay in the first place. Daily habits such as thorough brushing with fluoride toothpaste, flossing, limiting frequent sugary snacks, and staying hydrated help control plaque and reduce acid exposure to tooth surfaces. Professional services, including routine cleanings, topical fluoride applications, and targeted sealants, further protect enamel and occlusal surfaces that are most prone to cavities.
Regular dental exams enable early detection of enamel softening or small cavities when conservative measures can often halt progression, preserving more natural tooth structure. At Lorber Dental NY, PLLC, we emphasize prevention and individualized recall plans so patients receive the support and monitoring needed to maintain healthy, long-lasting smiles.
Quick Links