At the office of Lorber Dental NY, PLLC, we take a practical, prevention-first approach to oral health. Regular oral examinations are the cornerstone of that philosophy: they allow us to catch small problems before they become large ones, clarify individual risk factors, and help you preserve a comfortable, confident smile for years to come. Alongside clinical exams and professional cleanings, our team performs focused screenings for concerns such as oral cancer and periodontal disease and offers straightforward guidance on home care, diet, and habits that influence long-term outcomes.
Your initial appointment is designed to establish a clear baseline for your dental health and to make sure you feel heard. We begin with a careful review of your medical and dental history, asking about medications, prior procedures, and any symptoms or concerns you want addressed. This background helps us tailor the visit and identify factors—like dry mouth, certain medications, or previous dental work—that can affect treatment choices.
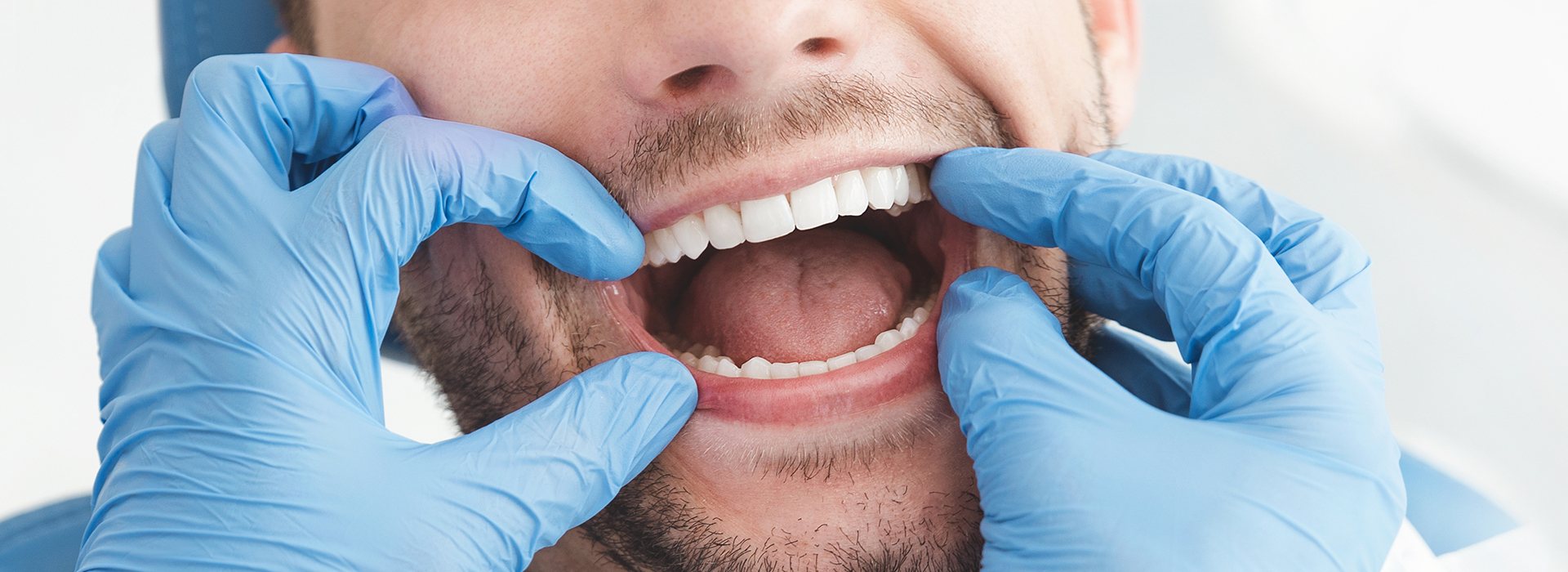
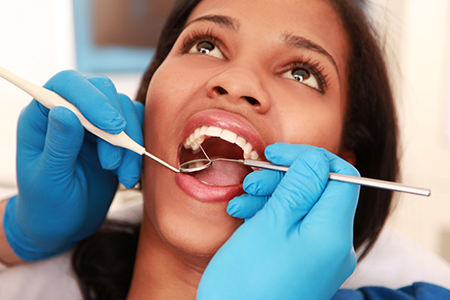
The clinical portion of the exam is methodical and transparent. The dentist and hygienist will inspect your teeth, gums, tongue, and the soft tissues of the mouth, and assess jaw function and bite alignment. We routinely include an oral cancer screening, a periodontal (gum) evaluation, and a look for signs of tooth wear from clenching or grinding. If needed, we’ll take targeted diagnostic images so nothing important is missed beneath the surface.
After the exam we review findings with you in plain language, prioritizing what matters most for your health and comfort. We’ll outline recommended next steps—whether that means a preventive treatment, a follow-up visit, or simply a refined at-home routine—and answer your questions so you leave with a clear plan. Our goal is to make the process collaborative and easy to understand.
The mouth is a window to the rest of the body. Many systemic conditions produce signs that appear in the oral cavity, and evidence increasingly shows that poor oral health can influence overall wellness. During a routine oral exam we look for clues—persistent gum inflammation, unusual lesions, or signs of infection—that may prompt closer medical evaluation or coordination with your physician.
The relationship goes both ways: illnesses such as diabetes, certain autoimmune conditions, and respiratory problems can affect saliva production, gum health, and healing. Noticing dry mouth, persistent bad breath, chronic sore spots, or unexplained gum changes during an exam can help us flag issues that merit further medical attention. Early detection and open communication about your health history make dental care safer and more effective.
Screenings we perform during an oral exam are intended to protect your mouth and support broader health. When we identify concerns, our recommendation will balance immediate dental needs with any potential systemic implications, helping you make informed decisions about next steps and referrals if necessary.

Consistent checkups paired with professional cleanings are the most effective strategy for preventing common dental problems. While daily brushing and flossing are critical, professional instruments and techniques remove hardened deposits and biofilm that are difficult to address at home. A thorough cleaning reduces inflammation, lowers the risk of cavities, and leaves your mouth feeling fresher and healthier.
Checkup visits also give us a chance to monitor changes over time. Detecting gum recession, early tooth decay, or shifting bite patterns in their earliest stages often means simpler, less invasive care. We also use these visits to coach patients on effective home care—demonstrating brushing and flossing techniques, recommending appropriate tools, and suggesting dietary adjustments that support long-term oral health.
Preventive care extends to all ages. For children we focus on building good habits and monitoring growth and development so that any need for orthodontic evaluation is identified early. For adults we tailor recall frequency and preventive measures to individual risk factors, aiming always to preserve natural teeth and avoid more extensive treatment when possible.
Visual inspection alone cannot reveal what lies beneath tooth surfaces and inside bone. Diagnostic imaging is an essential complement to the clinical exam because it uncovers hidden decay, the extent of bone support around teeth, and issues such as impacted or unerupted teeth. When used judiciously, radiographs provide critical information that guides safe and effective treatment planning.
Digital radiography has transformed how we capture and use images. Compared with older film methods, digital sensors require less radiation, produce images instantly, and allow us to enhance and share views with patients during the visit. Because images are stored electronically, they can be compared over time to monitor progression or improvement with treatment.
For complex cases—such as implant planning, impacted teeth, or detailed evaluation of jaw anatomy—three-dimensional cone beam CT (CBCT) imaging may be recommended. CBCT provides a layered, 3D perspective that helps clinicians plan procedures with precision and anticipate anatomic considerations that affect safety and outcomes.

Different images serve different diagnostic purposes. Bitewing radiographs are small, focused images that help detect decay between back teeth and show changes in bone level around those teeth. Periapical films capture the full length of individual teeth, revealing root tips and local bone health—information that’s helpful for diagnosing deep infections or planning root canal therapy.
A full-mouth series combines many small images to give a detailed record of all teeth and supporting structures and is useful when a comprehensive assessment is needed. Panoramic films produce a broad, two-dimensional overview of the jaws, teeth, and facial bones; they’re often used to evaluate erupting teeth, screen for large pathologies, and plan surgical procedures.
Cephalometric images provide profile views of the skull and jaws and are most commonly used in orthodontic assessment. When three-dimensional detail is required, CBCT delivers volume-based images that clarify bone architecture and spatial relationships. Your clinician will recommend the smallest, most appropriate set of images needed to answer clinical questions while keeping exposure low.
In summary, a thoughtful oral exam combines careful clinical evaluation, targeted imaging, and clear communication so you understand the findings and the options available. At Lorber Dental NY, PLLC we focus on prevention, early detection, and personalized recommendations to help you maintain a healthy, comfortable smile. Please contact us for more information or to schedule an examination.
A comprehensive oral exam is a systematic clinical evaluation of your teeth, gums, tongue, and the soft tissues of the mouth designed to establish a baseline for oral health. The exam typically includes an assessment of bite and jaw function, a periodontal check to evaluate gum health, and a screening for signs of oral cancer or unusual lesions. Clinicians also review your medical and dental history to identify risk factors that affect diagnosis and treatment planning.
When indicated, targeted diagnostic imaging such as bitewing or periapical radiographs is used to reveal decay between teeth or issues at the root that cannot be seen visually. The dentist and hygienist document findings and compare them to previous records when available to monitor changes over time. This coordinated approach helps prioritize preventive measures and determine whether further treatment or specialist referral is necessary.
Before your first oral exam bring a list of current medications, recent medical conditions, and any relevant dental records or x-rays if you have them. Avoid eating heavily right before the appointment so the clinician can assess breath and soft tissue without interference, and bring a list of questions or symptoms you want to address. If you experience dental anxiety, mention this when scheduling so the team can discuss comfort options and what to expect during the visit.
Arrive a few minutes early to complete any necessary registration or health history forms; providing accurate information helps the clinician tailor the exam to your needs. If you wear removable appliances such as dentures or clear aligners, bring them to the appointment so they can be evaluated for fit and hygiene. Clear communication about your habits, home care routine, and any changes in health improves the quality and safety of the exam.
Most patients benefit from routine exams and professional cleanings every six months because this frequency helps catch developing problems early and maintain gum health. Individuals with a history of periodontal disease, frequent cavities, dry mouth, or certain medical conditions may need more frequent visits, often every three to four months, to control risk factors and prevent progression. Your clinician will recommend a personalized recall interval based on your oral health status and risk profile.
Regular cleanings remove hardened deposits and biofilm that are difficult to remove at home and help reduce inflammation and the likelihood of future decay. Follow-up exams also allow the team to monitor changes in tooth wear, gum recession, or bite alignment and to adjust preventive care accordingly. Sticking to a recommended schedule is one of the most effective ways to preserve natural teeth and avoid more invasive treatment later.
During an oral exam clinicians routinely perform screenings for periodontal disease, oral cancer, and signs of tooth wear such as erosion or damage from clenching and grinding. The periodontal evaluation measures gum pocket depths, bleeding, and signs of attachment loss to determine whether active treatment or maintenance therapy is needed. An oral cancer screening includes a visual and tactile inspection of the lips, tongue, floor of the mouth, and other soft tissues for persistent sores, lumps, or discolorations.
Screenings may also include assessments of saliva flow, evaluation of removable appliances, and checks for indications of bruxism or temporomandibular joint dysfunction. When risk factors or suspicious findings are identified, the clinician will recommend targeted imaging, additional testing, or a referral to a medical specialist for further evaluation. This proactive approach helps detect problems early when treatment is simpler and outcomes are better.
Dental x-rays reveal conditions that cannot be seen during a visual exam, such as interproximal decay, the presence and extent of bone loss, and infections at the root tips of teeth. Different types of radiographs serve specific purposes: bitewings detect decay between posterior teeth, periapical images show the full tooth and surrounding bone, and panoramic films provide a broad overview of the jaws. Using the smallest, most appropriate set of images helps answer clinical questions while minimizing radiation exposure.
Digital radiography reduces radiation compared with older film techniques and produces images instantly, which can be enhanced and reviewed with the patient during the visit. For complex assessments such as implant planning or evaluation of impacted teeth, three-dimensional CBCT imaging may be recommended to clarify bone anatomy and spatial relationships. The goal is to combine clinical findings and imaging to create a safe, effective treatment plan tailored to each patient.
After the exam your clinician will review findings in plain language and outline prioritized next steps, which might include preventive care, restorative treatment, periodontal therapy, or a referral to a specialist. The team will explain the clinical reasoning behind each recommendation and discuss what to expect from follow-up procedures in terms of timing and clinical goals. This collaborative discussion helps you make informed decisions and address any concerns before starting treatment.
If additional diagnostic records are needed, such as more detailed imaging or impressions, those will be scheduled so that subsequent care can proceed with complete information. The practice will also advise on home care changes, behavioral modifications, or adjunctive therapies that support healing and long-term outcomes. Clear documentation and coordinated appointments help ensure continuity and effective management of identified issues.
The oral cavity often reflects broader systemic conditions, so routine oral exams can reveal clues such as persistent gum inflammation, unusual lesions, dry mouth, or delayed healing that may warrant medical investigation. Conditions like diabetes, certain autoimmune diseases, and nutritional deficiencies frequently manifest with oral signs that a dentist can recognize during an exam. When such findings arise, the dental team may recommend communication with your physician or suggest specific tests to evaluate potential systemic causes.
Recognizing these connections supports integrated care and can lead to earlier diagnosis or better management of underlying health issues. Dentists document observations and, when appropriate, provide referrals or written summaries to help coordinate care with other providers. Maintaining open communication about your overall health history and any new symptoms improves both dental and medical outcomes.
Oral exams for children focus on growth and development, early detection of decay, and establishing healthy habits that support long-term oral health. Pediatric assessments include monitoring eruption patterns, evaluating for early signs of malocclusion, and recommending preventive measures such as sealants or topical fluoride when appropriate. Exams also address guidance for diet, thumb-sucking or pacifier use, and home care techniques suited to a child’s age and dexterity.
For adults, exams emphasize periodontal health, restoration integrity, wear patterns, and screening for oral cancer and systemic-related oral signs. Recall frequency and preventive strategies are tailored to each patient’s risk factors, including medical conditions, medications, and lifestyle habits. Both pediatric and adult exams aim to prevent disease progression and preserve function and comfort across the lifespan.
The periodontal assessment measures pocket depths, bleeding on probing, and signs of attachment loss to determine the presence and severity of gum disease. If early-stage gingivitis is detected, the team focuses on thorough professional cleaning, improved home care instructions, and short-term monitoring to reverse inflammation. For established periodontitis, the clinician may recommend scaling and root planing, more frequent maintenance visits, or collaboration with a periodontist for advanced therapy.
Management always combines clinical treatment with patient-centered guidance on brushing, flossing, and lifestyle factors that influence gum health, such as smoking and diet. Regular reassessment after initial therapy helps determine treatment effectiveness and the appropriate long-term recall interval. The objective is to control infection, prevent further tissue loss, and maintain a stable, functional dentition.
You can schedule an oral exam by calling our office at (718) 913-8969 or by using the online appointment feature on our website during business hours. When you call, the team will ask about your availability, any symptoms or urgent concerns, and whether you are a new or existing patient so they can allocate the appropriate time for your visit. If you have recent dental records or x-rays from another provider, bring them or arrange to have them transferred to support a thorough evaluation.
The office of Lorber Dental NY, PLLC aims to accommodate new patients and emergency needs, and staff can explain preparation steps for your appointment when you schedule. Providing accurate medical history and a list of medications before the visit allows clinicians to tailor the exam safely and efficiently. If follow-up or specialist referral is recommended, the team will help coordinate next steps and answer any logistical questions you may have.
Quick Links