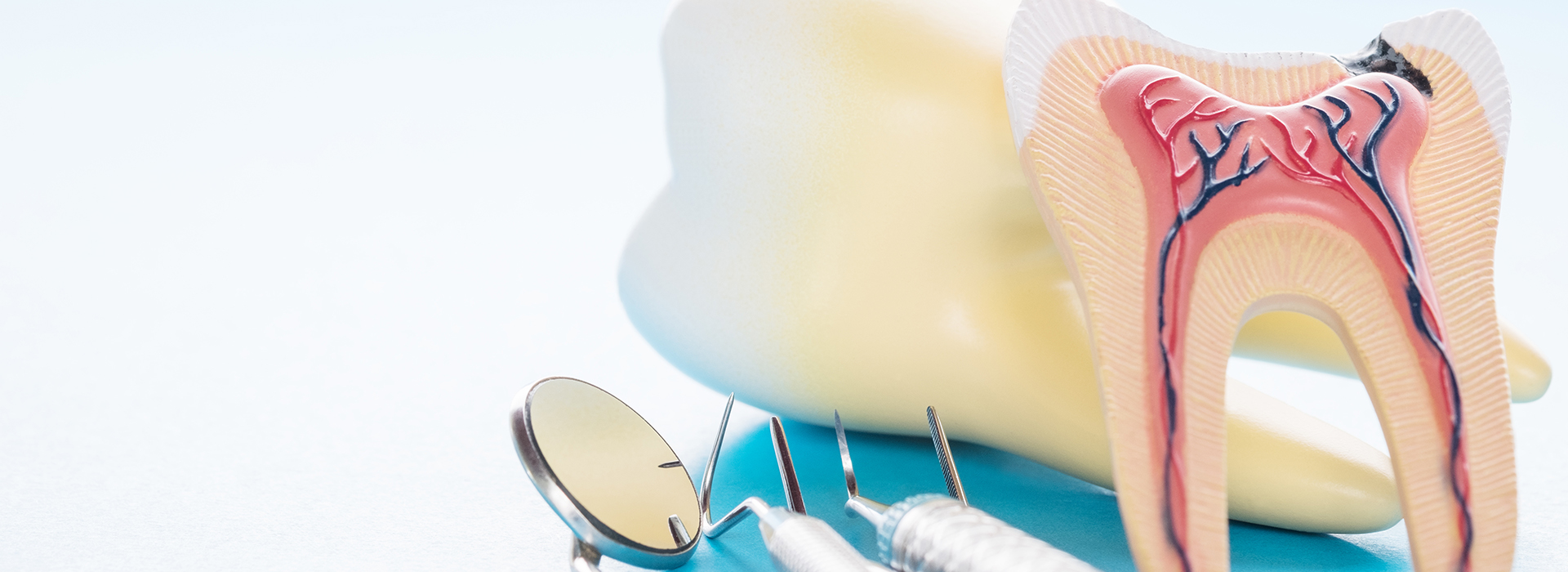
If a dentist recommends a root canal, it’s understandable to feel uneasy at first. Modern root canal therapy, however, is a refined, predictable treatment designed to stop pain, eliminate infection, and preserve your natural tooth whenever possible. Compared with extraction and replacement, root canal treatment often delivers the most natural, long-lasting outcome for biting, chewing, and the appearance of your smile.
At the office of Lorber Dental NY, PLLC, we combine gentle clinical technique, up-to-date imaging, and patient-centered care to make treatment as comfortable and efficient as possible. Our focus is on helping you regain oral health with clear explanations and a step-by-step plan tailored to your needs.
Saving a structurally sound tooth is usually better for long-term oral health than removing it. A tooth that remains in place helps maintain normal chewing patterns, supports surrounding teeth, and preserves bone in the jaw. When the inner tissues of a tooth (the pulp) become irreversibly damaged, root canal treatment removes the diseased tissue while keeping the outer tooth structure intact.
Contemporary endodontic techniques and materials have improved success and comfort. With proper restoration after treatment — typically a protective crown or onlay — many teeth treated with root canal therapy continue to function reliably for many years, often for the lifetime of the patient.
Choosing to preserve your natural tooth can reduce the need for more complex treatments later on. When a tooth is extracted, adjacent teeth may shift, and the long-term solution often involves prosthetic replacements such as implants or bridges. Whenever feasible, root canal therapy is the conservative choice to maintain your natural dentition and oral function.

Inside each tooth is a central chamber that contains connective tissue, tiny blood vessels, and nerve fibers — collectively called the dental pulp. The pulp helps a developing tooth grow and, even after full development, gives early warning signals when something goes wrong. When that tissue becomes infected or severely inflamed, it can no longer recover on its own.
Several events can lead to pulp damage: deep decay that reaches the inner chamber, a crack or fracture that exposes the nerve, trauma from an injury, or repeated restorative work on the same tooth. Sometimes the tissue becomes compromised without dramatic symptoms, which is why routine exams and X-rays are important.
When the pulp is affected, patients may notice symptoms that indicate the need for evaluation. Early treatment limits the spread of infection and preserves more of the natural tooth. In many cases, prompt root canal therapy prevents more extensive problems and restores comfort.
Although every patient’s course is different, a thorough clinical exam and radiographic assessment will determine whether root canal therapy is the most appropriate option to save the tooth.
Although not every instance of dental discomfort indicates the need for root canal therapy, some of the warning signs that you might require this procedure include the following:
Continuous or throbbing pain that doesn’t resolve with over-the-counter measures often signals an internal problem. Pain that wakes you from sleep or intensifies over time is a common reason patients seek urgent evaluation.
Discomfort when consuming hot or cold foods and beverages — especially when it lingers after the stimulus is removed — can indicate inflammation or nerve damage within the tooth.
Sharp discomfort while chewing or tenderness to light pressure often points to pulpal involvement or a developing infection that affects the tooth’s supporting tissues.
A single tooth that becomes noticeably darker than the others may have internal changes following trauma or longstanding injury to the pulp. This can be a sign that the tissue inside has deteriorated.
Structural damage can expose the inner tooth and allow bacteria to reach the pulp. Even small fractures sometimes permit microbes to enter, leading to inflammation and infection.
Localized gum swelling, a tender lump, or pus drainage near a tooth usually indicates an active infection. Prompt assessment is important to control the problem and prevent it from spreading.
Infection or advanced breakdown around a root can reduce the bone support for a tooth, causing mobility. Successful root canal therapy, combined with appropriate restoration, can often halt and reverse this process as healing occurs.
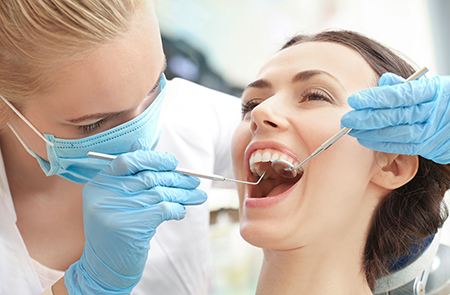
Early diagnosis and treatment improve the likelihood of saving a tooth. Some teeth show no obvious symptoms at first and are discovered during routine exams or X-rays. When detected early, infections are easier to manage and less likely to damage surrounding structures.
Delaying care can allow an infection to progress, producing more pain, bone loss around the root, or spread to adjacent teeth. In some cases, a delay increases the chance that a tooth will be lost instead of being salvaged. Timely evaluation allows your dental team to recommend the most conservative and effective path forward.
Your dentist will use clinical testing and imaging to determine the extent of the problem and whether root canal treatment is indicated. When necessary, additional consultations with a specialist may be recommended to ensure the best outcome for complex anatomy or difficult cases.
Thanks to local anesthesia, modern instruments, and refined techniques, most root canal procedures are performed with minimal discomfort. Care begins with sterile isolation and numbing of the area so you remain comfortable throughout the procedure.
After accessing the inner chamber, the dentist gently removes the diseased or infected pulp, cleans and shapes the root canals, and disinfects the space. The canals are then filled with a biocompatible material to seal them and prevent reinfection. A temporary filling is placed while the tooth heals and until a permanent restoration can be completed.
Some treatments are finished in a single visit, while others require two appointments — for example, teeth with complex canal anatomy or active infections that benefit from interim medication. If you experience significant anxiety, sedation options are available to help you remain relaxed during care.
After treatment you may feel some tenderness for a few days as surrounding tissues recover. Any lingering numbness from anesthesia typically subsides within a couple of hours. Our team will advise on appropriate comfort measures and when it is safe to resume normal eating and activity.
If antibiotics or other medications are prescribed, it is important to follow the instructions provided. You should also protect the treated tooth from heavy biting forces until a permanent crown or restoration is placed; this helps prevent fracture and preserves the long-term success of the treatment.
Good oral hygiene and regular dental visits are essential to the longevity of the treated tooth. With proper restoration and routine care, a tooth that has received root canal therapy can remain healthy and functional for many years.
At our office, we’re committed to clear communication and attentive follow-up care. If you notice persistent discomfort, swelling, or any new symptoms after treatment, contact our team so we can assess and address your needs promptly.
In summary, root canal therapy is a reliable, tooth-preserving procedure that relieves pain, removes infection, and restores function. If you think you may need evaluation or would like more information about root canal treatment, please contact us for further assistance.
A root canal is a dental procedure that removes infected or damaged pulp from inside a tooth and seals the canal to prevent reinfection. It preserves the outer tooth structure so patients can maintain normal chewing function and a natural appearance. Dentists recommend root canal therapy when pulp tissue cannot recover on its own and infection or severe inflammation threatens the tooth.
Modern root canal treatment uses precise instruments, effective local anesthesia, and sterilization techniques to make the procedure predictable and comfortable for most patients. With proper restoration after the procedure, many treated teeth continue to function for years and often for a lifetime. Early diagnosis and prompt treatment increase the chance of saving the natural tooth and avoiding more extensive procedures later on.
The dental pulp can become damaged or infected for several reasons, including deep decay that reaches the inner chamber, a cracked or fractured tooth, or traumatic injury that compromises blood supply. Repeated restorative procedures on the same tooth or undetected microfractures can also permit bacteria to reach the pulp. Once bacteria or inflammation takes hold, the tissue often cannot repair itself and requires professional treatment.
Sometimes pulp damage develops slowly and without obvious symptoms, which is why routine exams and X-rays are important for early detection. Left untreated, an infected pulp can lead to abscess formation, bone loss around the root, and spread of infection to adjacent teeth or tissues. Timely evaluation allows your dental team to recommend the most conservative and effective treatment to preserve oral health.
Symptoms that commonly signal the need for evaluation include persistent, severe toothache that may be throbbing or sharp, especially when it wakes you at night. Heightened sensitivity to hot or cold that lingers after the stimulus is removed and pain when biting or applying pressure are frequent warning signs. A single tooth that darkens in color, localized gum swelling, or a small pimple-like bump on the gum may also indicate underlying pulp disease.
Not every tooth with discomfort requires a root canal, but these signs warrant prompt clinical and radiographic assessment to determine the cause. Early diagnosis limits the spread of infection and increases the chances of a successful, tooth-preserving outcome. If you experience severe pain, swelling, or drainage near a tooth, contact your dental office for an urgent evaluation.
A modern root canal procedure begins with numbing the area using local anesthesia and isolating the tooth to maintain a sterile field, typically with a rubber dam. The clinician creates a small access opening to reach the pulp chamber and gently removes the diseased tissue with specialized instruments. The canals are shaped, cleaned, and disinfected to eliminate bacteria and debris before being filled to seal the space.
After the canal system is sealed with a biocompatible material, a temporary filling is placed while the tooth heals and a definitive restoration is planned to protect the remaining structure. Some cases are completed in a single visit, while teeth with complex anatomy or active infections may benefit from interim medication and a second appointment. At the office of Lorber Dental NY, PLLC we use up-to-date imaging and gentle techniques to tailor each treatment to the individual needs of patients.
Most patients experience little to no pain during a root canal because local anesthesia effectively numbs the tooth and surrounding tissues. Modern instruments and techniques further reduce discomfort, allowing clinicians to work precisely and efficiently. If anxiety is a concern, sedation options can be discussed to help patients remain calm throughout the procedure.
Mild tenderness or sensitivity around the treated tooth is common for a few days as surrounding tissues recover, and over-the-counter analgesics usually control this discomfort. It is important to follow post-treatment instructions and avoid chewing on the tooth until a permanent restoration is placed to prevent fracture. Contact your dental team if pain intensifies, swelling develops, or symptoms persist, as additional care may be necessary.
Root canal therapy can often be completed in a single appointment, but some situations call for two visits, such as complex canal systems or cases where an antibacterial dressing is needed between appointments. Your dentist will decide the best approach based on clinical findings, radiographic evidence, and the tooth's anatomy. When treatment is spread over multiple visits, the clinician will place a sealed temporary restoration to protect the tooth between appointments.
Follow-up visits also allow the dentist to confirm healing and coordinate the final restoration, which is essential for long-term success. If symptoms recur or a previous root canal becomes symptomatic, retreatment or referral to a specialist may be recommended to address persistent or recurrent infection. Regular dental exams and X-rays help monitor the treated tooth and surrounding structures over time.
After root canal therapy, many teeth benefit from a protective restoration — commonly a crown or onlay — to reinforce the remaining tooth structure and restore normal function. Teeth that have lost significant enamel or dentin are more likely to fracture without a full-coverage restoration. The timing of the final restoration depends on the extent of treatment and the clinician's judgment to ensure a durable, sealed tooth.
A well-fitted crown or onlay distributes biting forces evenly and helps prevent recurrent decay around the margins of the restoration. During the restorative phase your dentist will check the bite and make adjustments as needed to maintain comfort and function. With appropriate restoration and routine care, a treated tooth can provide reliable service for many years.
The main alternative to root canal therapy is extracting the affected tooth and replacing it with a prosthetic option such as an implant, bridge, or removable partial denture. Extraction removes the source of infection but also sacrifices the natural tooth and may lead to changes in chewing dynamics and neighboring tooth position over time. Choosing between saving a tooth and extracting it involves evaluating the remaining tooth structure, periodontal condition, and overall oral health.
When possible, preserving the natural tooth with root canal therapy is often the more conservative choice that maintains jawbone support and natural chewing patterns. Your dental team will review the risks and benefits of each option and help you select the solution that best meets your functional and clinical needs. Complex cases may warrant consultation with a restorative dentist or implant specialist to plan the most appropriate long-term outcome.
Referral to an endodontist, a dentist who specializes in root canal therapy, may be recommended for teeth with complex canal anatomy, prior root canal failure, or difficult access. Endodontists receive additional training and use advanced techniques to manage challenging cases, perform retreatments, and treat teeth with unusual anatomy. Your general dentist will consider a specialist referral when it increases the likelihood of a successful, tooth-preserving result.
You should also seek specialist care if a previous root canal does not resolve symptoms or if imaging shows persistent infection around the root tip. In some cases apical surgery or endodontic microsurgery performed by a specialist can address issues not resolvable through non-surgical retreatment. Prompt referral and collaboration between providers help ensure the best possible prognosis for compromised teeth.
Preventing the need for a root canal centers on good daily oral hygiene, including thorough brushing, flossing, and regular professional cleanings to limit decay and gum disease. Early treatment of cavities, timely repair of cracked or chipped teeth, and use of protective devices like mouthguards for sports reduce the risk of pulp damage. Avoiding excessive forces on teeth, such as chewing ice or hard objects, also helps protect enamel and dentin from fractures that can lead to infection.
Routine dental exams with appropriate X-rays allow your dental team to detect problems before they reach the pulp, increasing options for conservative care. If you notice any persistent sensitivity, darkening of a tooth, or swelling around a tooth, seek prompt evaluation to limit progression and preserve tooth structure. These preventive steps support long-term oral health and decrease the likelihood of needing complex treatments in the future.
Quick Links